Vancouver surgeons to herald new era in lung transplant
Credit to Author: Pamela Fayerman| Date: Thu, 15 Aug 2019 07:01:34 +0000
The kind of lungs that were considered unsuitable for transplant will now get a shot at saving lives as medical experts at Vancouver General Hospital introduce a new high-tech process called ex vivo lung perfusion.
Health professionals at VGH have been practising for weeks on human, but unusable, lungs donated for research. On Friday, they will finish their training and certification on the new equipment. That means the first transplant utilizing the new high-tech equipment could occur as early as this weekend.
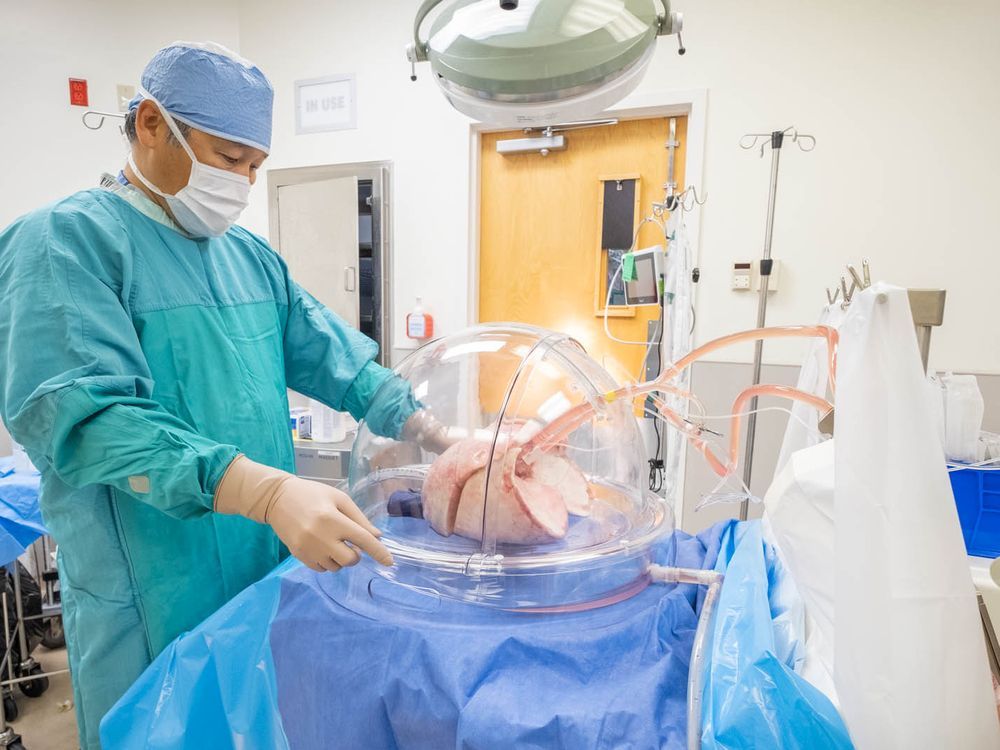
The ex vivo lung perfusion process lets transplant experts treat lungs as they sit in a humidified, dome-shaped “organ chamber” connected by tubes to machinery that pumps in nutrients like fluids, proteins and oxygen. It also allows health professionals to determine the quality of donor lungs through physical examination and imaging studies to rule out tumours, embolisms and lung diseases while sustaining the lungs in an environment that mimics the human body.
Problems like infections, pneumonia, edema (excess fluid retention) and inflammation are some of the conditions that can be treated to improve the quality of the donor lungs.
Those that can’t be fixed while hooked up to the machinery won’t be used for transplant, “thereby sparing patients the potentially deadly consequences of implanting failing organs that won’t function properly,” said Dr. John Yee, a thoracic surgeon who is the director of the B.C. Lung Transplant Program.
Dr. John Yee examines a donor lung in the dome of the new $325,000 Ex Vivo lung perfusion machine at VGH.
“Right now, the main emphasis is for us to test-drive the lungs to ensure they’re going to work. Using this technology is going to help make transplantation safer, and to convert organs that are marginally usable into organs that are definitely and reliably usable,” Yee said.
He said the new method for examining lungs is expected to increase the number of lungs available for transplant by about 20 per cent, while improving outcomes for recipients after transplantation.
Based on data from the past 28 years, about 70 per cent of patients who get a double-lung transplant can expect to live at least another five to 10 years. Yee said patients are within a year or two of death by the time they get to the top of the transplant list, so the transplant buys many of them years of life.
He hopes the new equipment — by allowing use of more donor lungs — will mean an end to people dying while on the waiting list.
While single lung transplants were fairly standard several years ago, Yee said the transition to nearly all double lung transplants occurred as more organs became available.
“Having a double lung is like having a car with two tanks of gas instead of one. It will go further,” he said, adding that starting off with two new lungs prolongs the time to infection or rejection.
Lung transplant teams at Vancouver General Hospital are wrapping up training on their new $325,000 ex vivo lung perfusion equipment.
Lung transplants have been done in Canada since the 1980s, but studies have shown that only 15 to 20 per cent of donor lungs are reliably safe and effectively used. By contrast, the rate of use for donor hearts is 30 per cent. Over the past few years in B.C., about 50 lung transplants have been done each year. But at any time, dozens of people are waiting.
Yee said typical donors are individuals who’ve been in accidents, had a brain hemorrhage or had a drug overdose. Often, during the resuscitation process, their lungs filled with fluids and developed pneumonia while on mechanical ventilators, a hospital-acquired injury. Until now, lungs from such patients may have been considered too risky to use. The new equipment, Yee said, gives transplant team experts a four- to six-hour window to examine and recondition the lungs.
He expects the equipment will be used six to 10 times a year on lungs that are initially considered “marginally usable.”
B.C. is one of only four provinces offering a lung transplant program; the others are Alberta, Ontario and Quebec.
Yee said implanting lungs is serious business and “not something that we would promote or take lightly. … There are a lot of consequences, like drugs that patients have to take for the rest of their lives to prevent rejection and susceptibility to infections.”
Pulmonary fibrosis is a common disease that can lead to a lung transplant and, in the past few years, VGH has disclosed some spectacular success stories in patients with that disease and other potentially fatal lung conditions.
While deaths after fentanyl and other drug overdoses have meant a bigger supply of some organs for transplant, Yee said it hasn’t been as much of a factor in lung transplants.
“The opioid epidemic has been a huge social tragedy. … But it hasn’t really helped us for organ retrieval because many of these lungs are too damaged by the time these victims have been found dead. Their lungs are often not viable, they aren’t salvageable. It’s a different story for kidneys and livers. But the lungs are more finicky. They are the most difficult to accomplish transplants successfully.”
B.C. Transplant has been studying various ways to increase lung transplants through various previously unthinkable routes: allowing donations from euthanasia patients and from individuals infected with hepatitis C. In Toronto, where doctors pioneered the ex vivo system, research has shown that it is safe to use lungs from hep C donors. After their lungs are removed, the organs can be treated in the domed system to knock out the virus before being transplanted.
B.C. Transplant has so far allowed only kidney transplants from hep C-infected donors into non-Hep C recipients since there is now an effective treatment that can be given to organ recipients. No other organ transplants involving Hep C infected donors have been done to date.
To register to be an organ donor, click here.
pfayerman@postmedia.com
Twitter: @MedicineMatters